Demedicalize Architecture
Text by Giovanna Borasi and Mirko Zardini
We live in a state of pervasive anxiety. Every day, we are confronted with problems stemming from the energy crisis, the use of natural resources, pollution, decreasing biodiversity, climate change, new epidemics, the harmful effects of industrial production processes, and our consumerist lifestyles. We perceive our bodies as constantly at risk (from sources difficult to pinpoint) of contamination and disease. This increasing concern and obsession with health and well-being, mainly among urban populations in the West, is triggering an inevitable process of medicalization: a process in which ordinary problems are defined in medical terms and understood through a medical framework. As medical sociologist Peter Conrad has written,
In the 1970s, the terrain of health and illness looked quite different from what we find in the early twenty-first century.... Neither obesity nor alcoholism was widely viewed in the medical profession as a disease…[and] medical professionals have [since] identified several problems that have become commonly known illnesses or disorders.1
Today, our bodies are the subject and ultimate object of consumption. Health has become the number one priority as our faith in the steady progress and improvement of society at large erodes, giving way to lingering feelings of uncertainty and fear. We are so carried away by the idea of health that we have created a new moralistic philosophy: healthism.2 We place our trust in medicine and its promise of rational, scientific solutions, forgetting what Ivan Illich noted in Limits to Medicine back in 1976, that no cure is “value free”: “Medicine is a moral enterprise and therefore inevitably gives content to good and evil. In every society, medicine, like law and religion, defines what is normal, proper or desirable.”3
Read more
Our health-obsessed society, however, offers diverse interpretations of health. For example, the idea of health is no longer identified primarily with the absence of illness, but has expanded to include a state of general well-being concerning all types of functioning, from physical and biological to social and cultural. Nevertheless, the ambition for total well-being is fragmented and parcelled out in a series of policies and disconnected actions. The means to overcome old and new illnesses, the production of a new, healthier body to withstand (inevitable) deterioration, is today achieved through voluntary biomedical technology and individual efforts (“staying in shape”), supported by new environmental urban planning policies.
The distinction between a sick body and a sound body has also grown. Being in good health today seems to imply youth and athleticism. A healthy body is part of a new aesthetic and erotic ideal, the product of concurrent medical trends, health policies, and individual choices, as medical historian Dorothy Porter has observed.4 We are far from the welfare-state health policies that were developed during the postwar era to promote preventive medicine and establish good health as a social right of every citizen, in keeping with studies by British sociologist Thomas Humphrey Marshall from the 1950s.5 Higher health care costs, reduced public services and spending, and the affirmation of an individualist rhetoric mean that today, health is increasingly considered an individual responsibility.
Contemporary architecture and urban planning seem to address, uncritically, the conditions and context in which this discourse on health is developing. In most cases, design disciplines prefer to rely on an abstracted, scientific notion of health, and very literally adopt concepts such as “population,” “community,” “citizen,” “nature,” “green,” “development,” “city,” and “body” into a professionalized, disciplinary discourse that simply echoes the ambiguities characteristic of current debate. Contemporary practitioners also prefer to ignore the fact that economic processes are closely intertwined with environmental processes and especially that concepts of the body, health, and sickness are products of history, politics, economics, and culture. To attempt to properly “diagnose” related problems of urbanism, we must not speak of health in abstract terms, but rather of various ideas and states of health. As Jonathan M. Metzl has noted, “‘Health’ is a term replete with value judgments, hierarchies and blind assumptions that speak as much about power and privilege as they do about well-being. Health is a desired state, but it is also a prescribed state and an ideological position.”6
The Imperfect Health project does not represent a comprehensive survey of the relationships between health, architecture, cities, and the environment. On the contrary, it draws on projects and texts meant to highlight some of the uncertainties and contradictions present in ideas of health and health care that are emerging in Western countries today, particularly in Europe and North America.
Some projects still adhere to the modernist vision of architecture and urban planning as rational processes that provide possible treatments for old and new illnesses, and are even capable of producing new bodies. But other failed experiments of the twentieth century provide enough evidence to suggest that architecture, urban planning, and landscape architecture should also exercise caution, giving more attentive consideration to possible effects and outcomes. The unexpected (often unhealthy) consequences of what had been celebrated as progress—the triumphs of industrial production—are increasingly evident. It is not only a question of damage done to the environment by polluting land, air, and sea. An absolute confidence in the ability to provide perfect solutions can easily give way to its polar opposite: doubt, and the consequent emotions of anxiety and fear. In the particular case of asbestos, for example, what was once regarded an ideal material for every imaginable application is today pronounced highly carcinogenic. Paradoxically, Imperfect Health tells of an unavoidable process of defeat: the inability of architecture to offer an optimal or permanent fix based on its promise of rational parameters.
Machiavelli long ago observed, “In the order of things it is found that one never seeks to avoid one inconvenience without running into another; but prudence consists in knowing how to recognize the qualities of inconveniences, and in picking the less bad as good.”7 Given these complex conditions of engagement, it is critical that the relationship between architecture and health be revised. While perhaps partly responsible, architecture is not always capable of providing positive solutions for the environment or the “sick” body. Instead, a confused and anxious contemporary architecture struggles to produce new manifestations that avoid exalting the spectacle of capital of the last twenty years. While architecture is looking once again into the ambiguous political, cultural, moral, and, above all, social ideas of health and medicalization for both justification and a new mandate, it should seek to challenge—rather than pacify—the newly emerging neo-liberal agenda and question a medicalized vision and approach toward health issues.
-
Peter Conrad, The Medicalization of Society: On the Transformation of Human Conditions into Treatable Disorders (Baltimore: Johns Hopkins University Press, 2007), 3. ↩
-
Jonathan M. Metzl and Anna Kirkland, eds., Against Health: How Health Became the New Morality (New York and London: NYU Press, 2010). ↩
-
Ivan Illich, Limits to Medicine. Medical Nemesis: The Expropriation of Health (London: Marion Boyars, 1976–2010), 45. Significantly, Ivan Illich and Michel Foucault, contemporary philosophers both born in 1926, developed the most in-depth critique of medicine and the process of medicalization during the 1970s. ↩
-
Dorothy Porter, Health, Civilization and the State: A History of Public Health from Ancient to Modern Times (London: Routledge, 1999). ↩
-
Ibid., 233. ↩
-
Metzl and Kirkland, Against Health, 1–2. ↩
-
Niccolo Machiavelli, The Prince (1532; Chicago: The University of Chicago Press, 1985 and 1998), 91. ↩
Cure or care
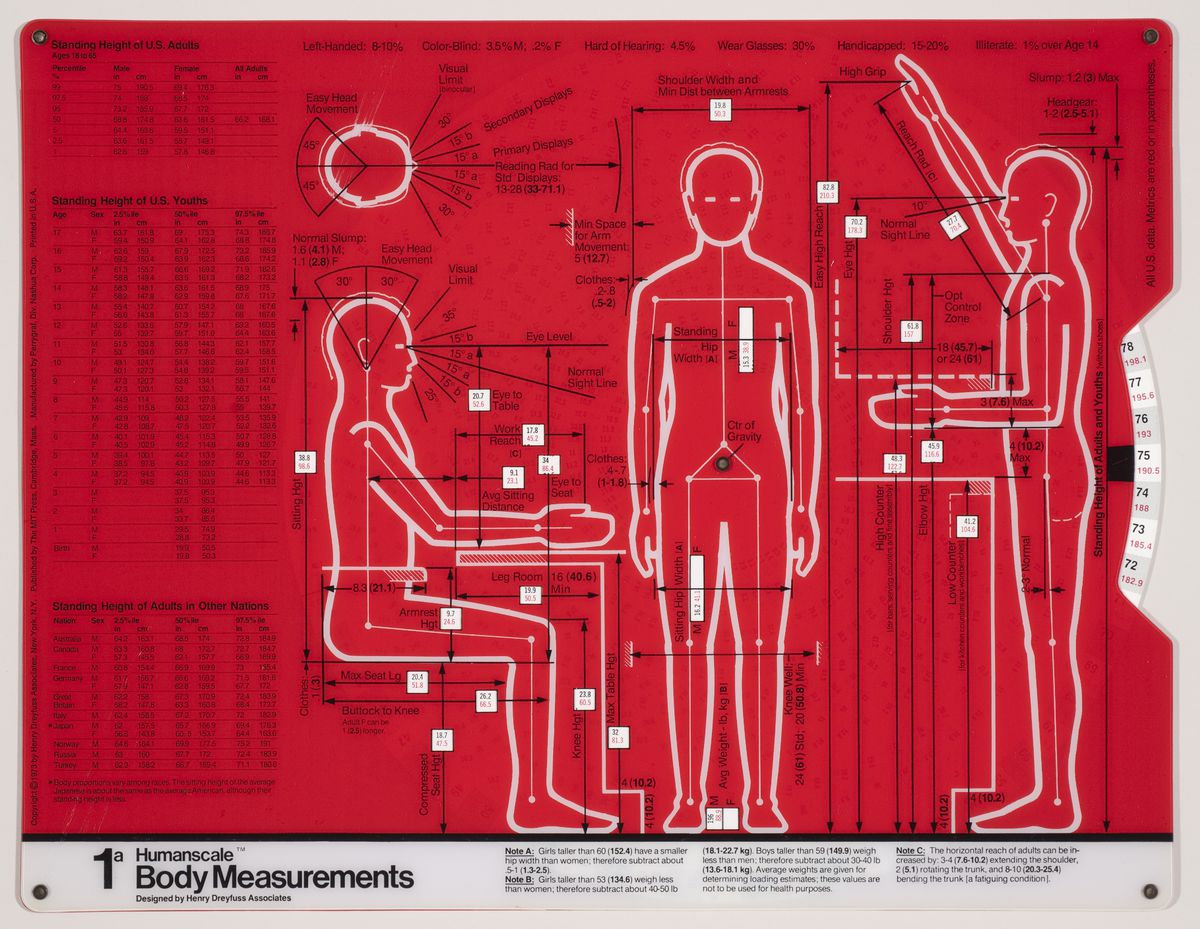
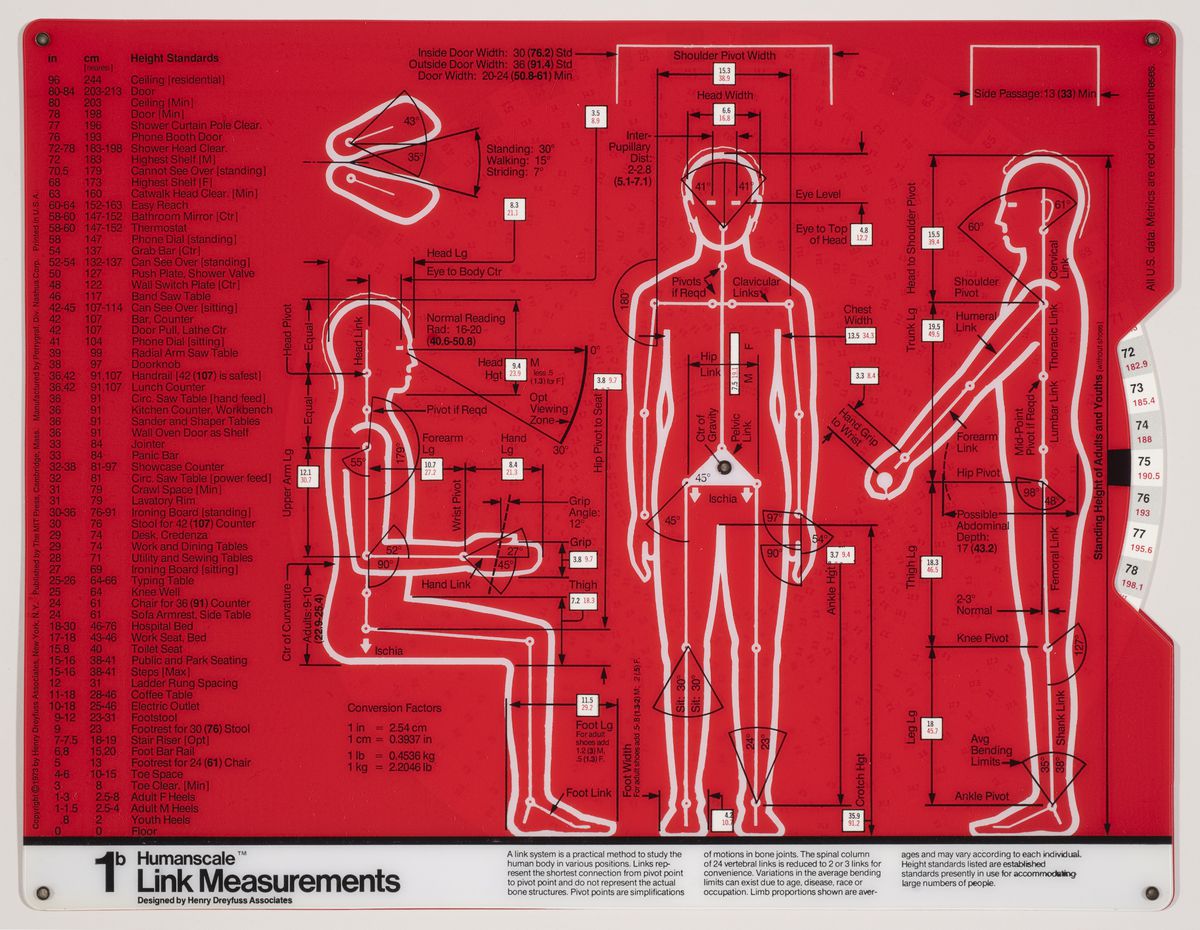
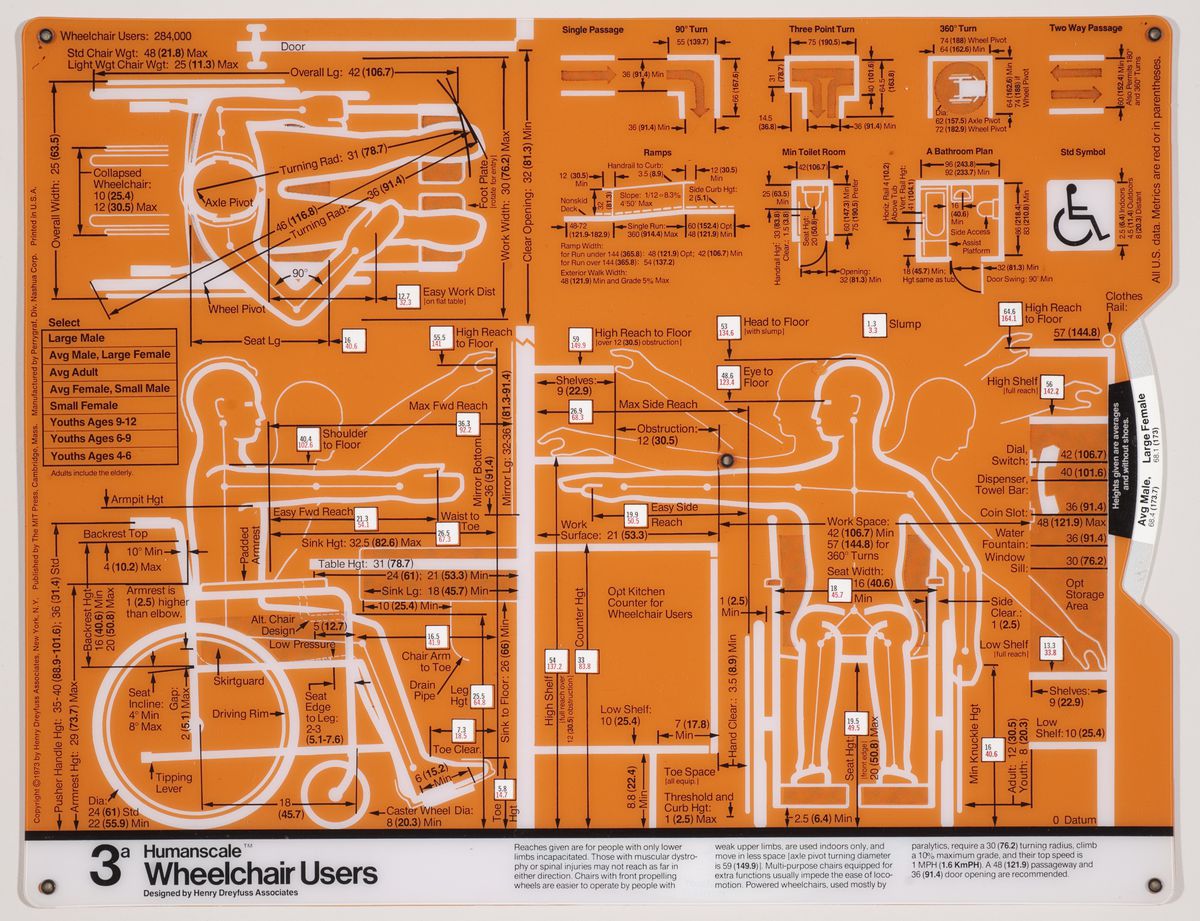
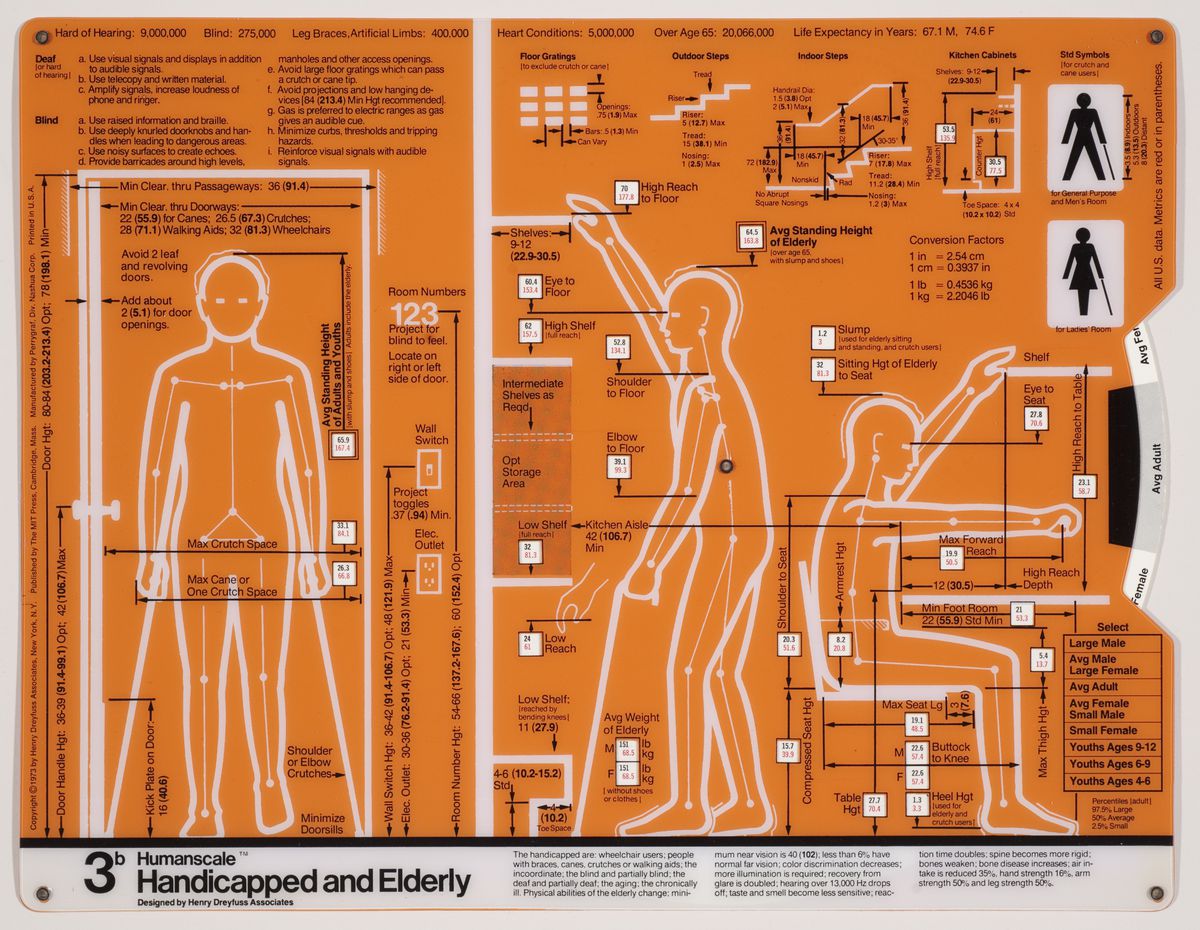
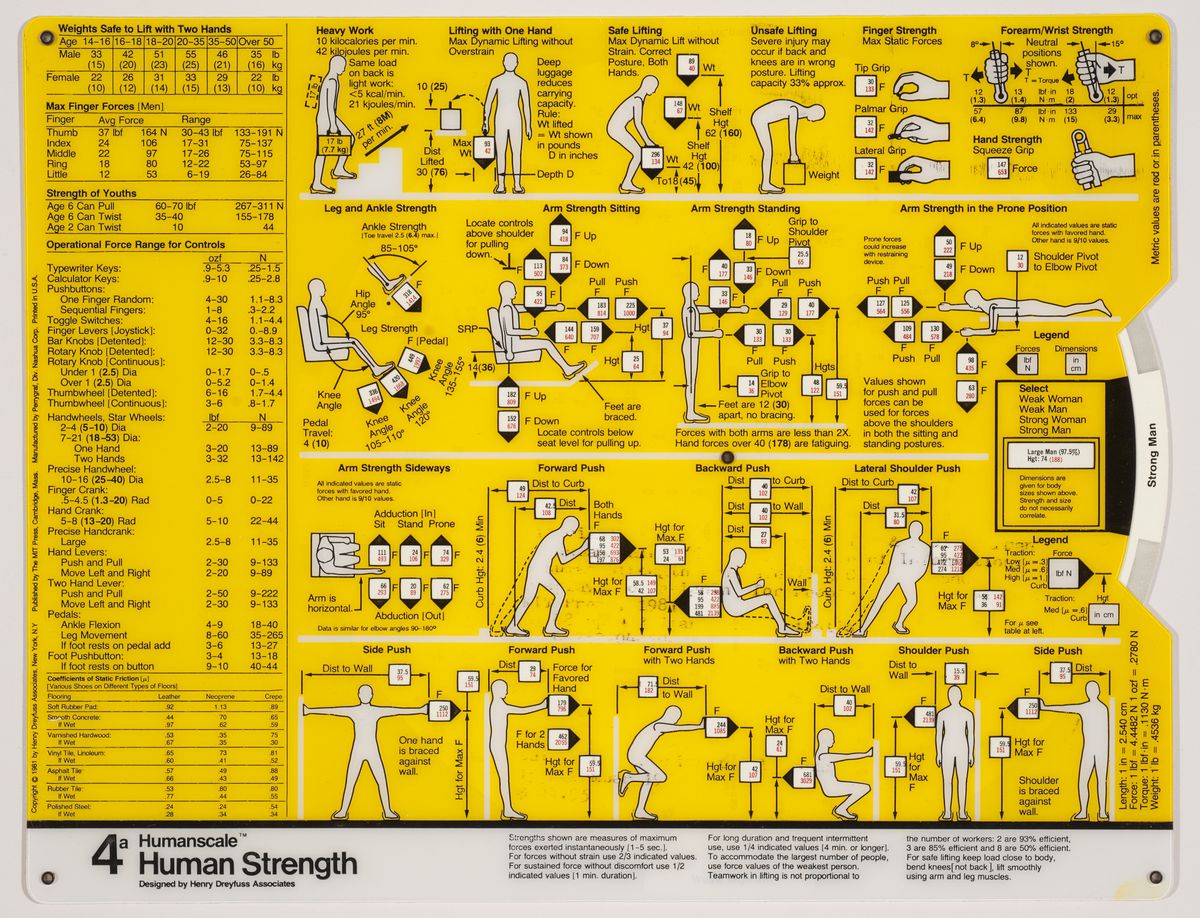
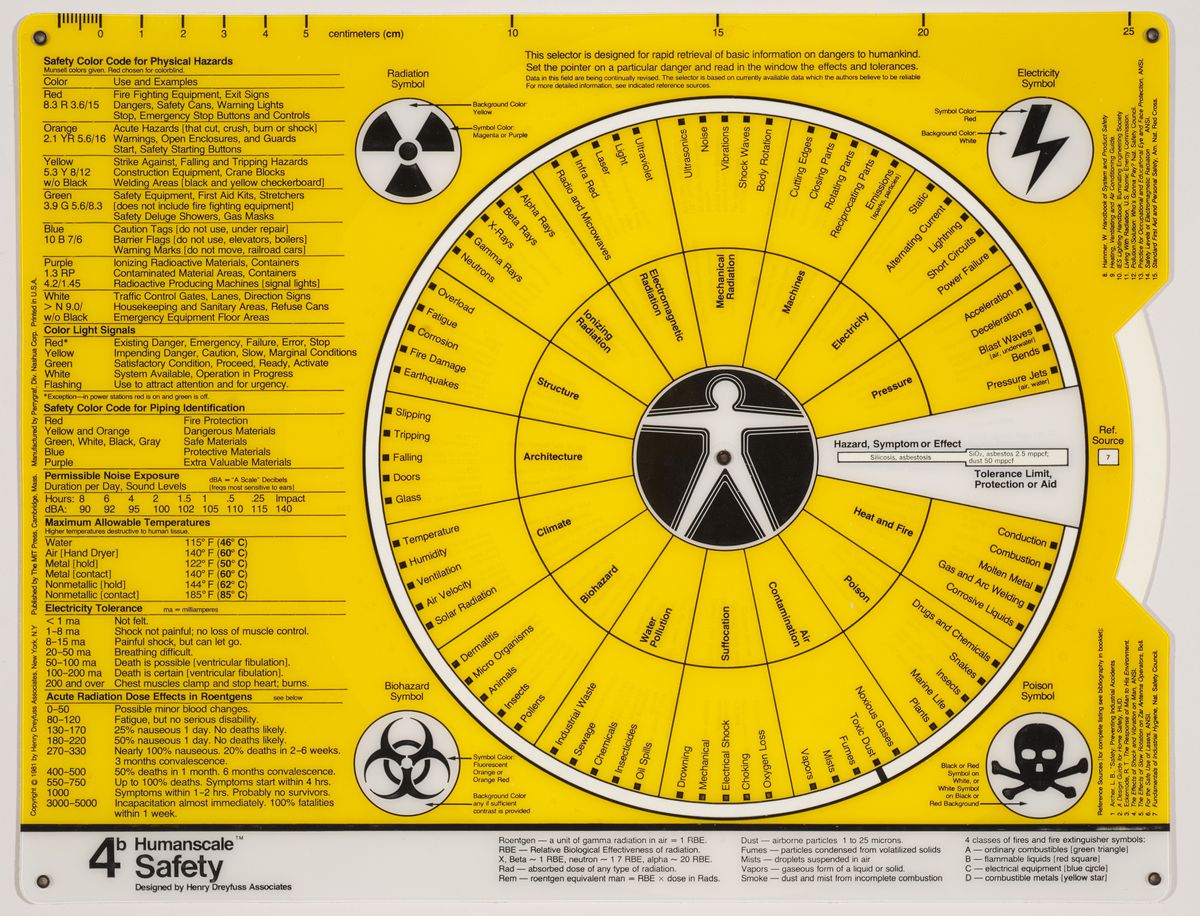
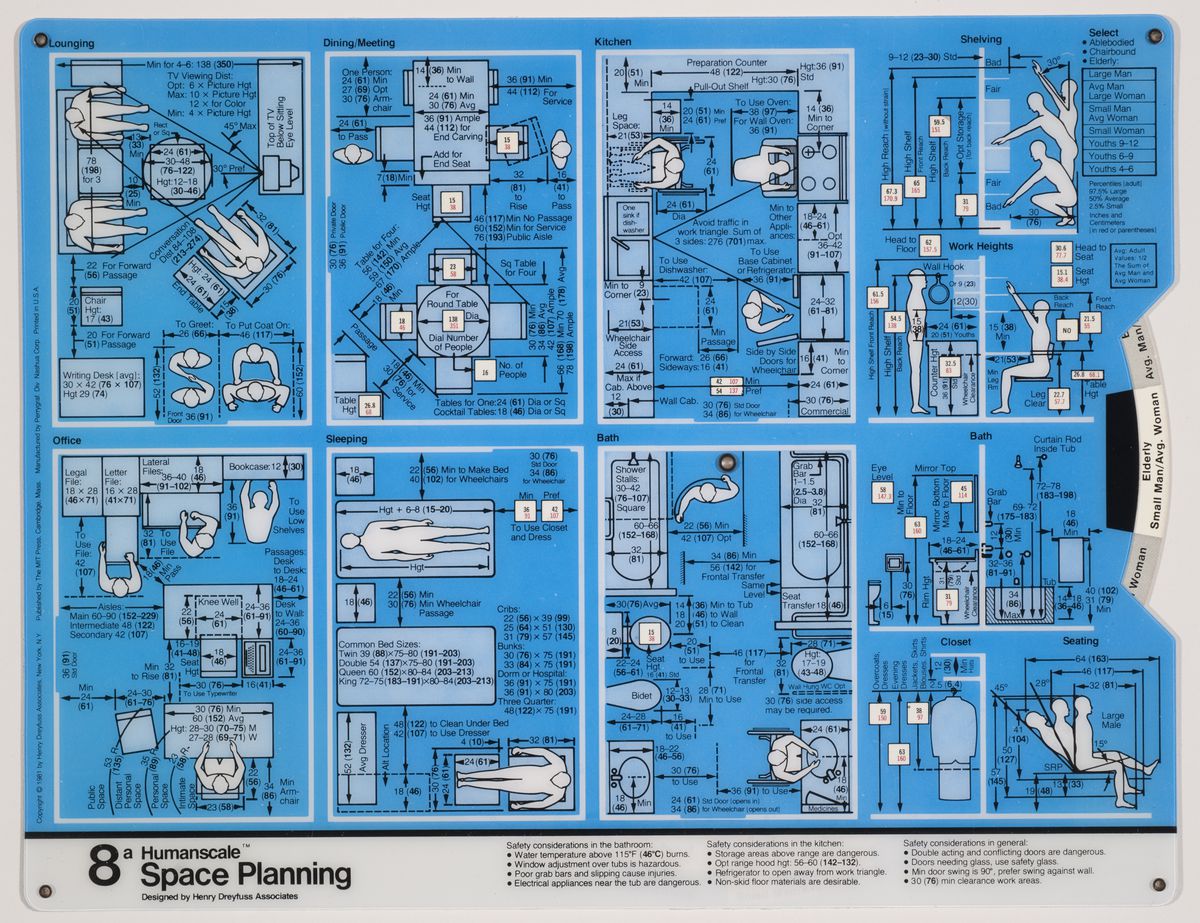
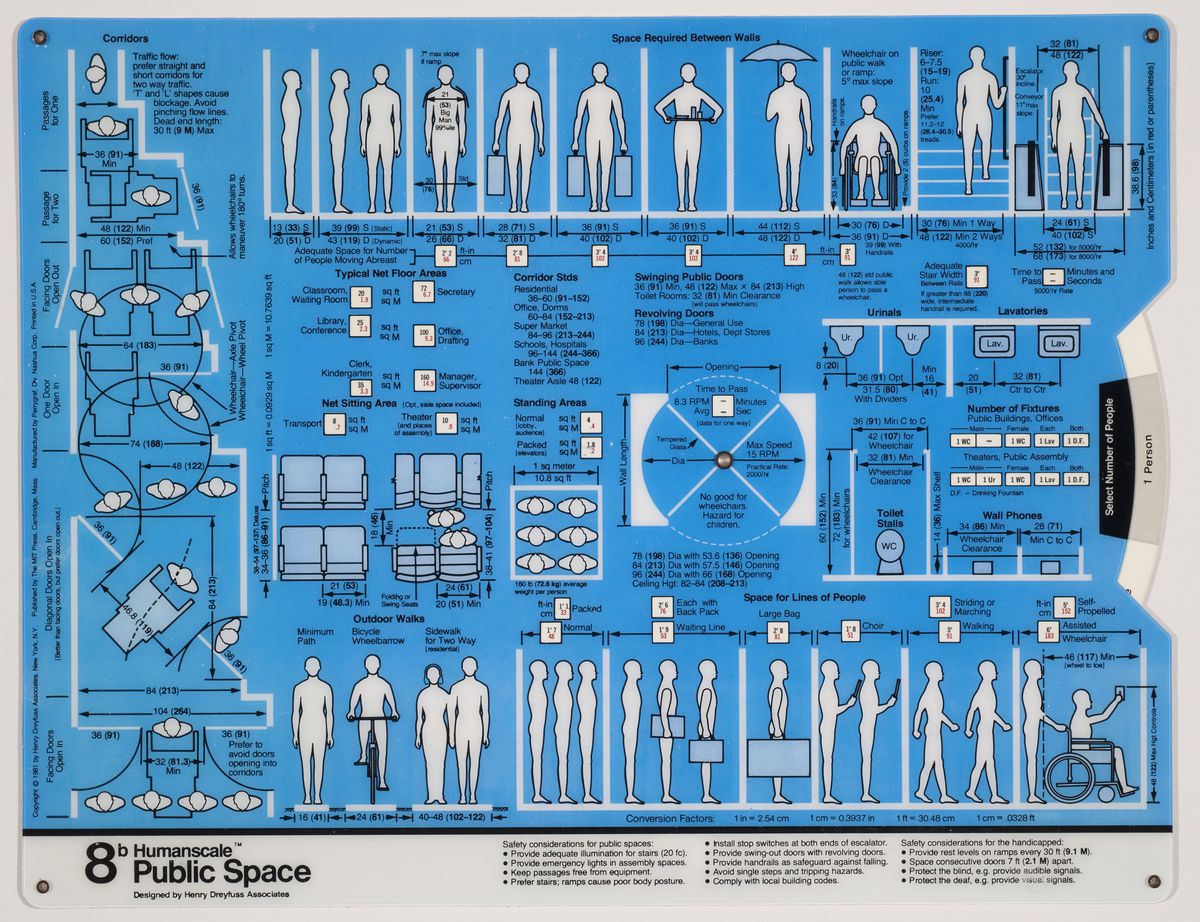
The size and characteristics of the body we inhabit today are very different from those of a century ago, or even a half-century ago. Anthropometric measurements first indicated by industrial designer Henry Dreyfuss in the late 1950s no longer seem to satisfy contemporary shapes. Dimensions have changed so much that various projects are underway to scan the new male body, for example, so as to properly define men’s clothing sizes. According to fashion manager Umberto Angeloni, “Traditional men’s sizes derive from measurements taken at the time of the Second World War, when men were very different.... We are still trying to dress men of the third millennium according to the bodies of their grandfathers.”1
Meanwhile, physical and athletic performance has improved. Life expectancy is longer, particularly in Europe, Japan, and North America, distinguishing these regions and cultures from the rest of the world. Building a different body not only prolongs life but also produces a new humanity, with new concerns and values. We think about family and sex differently and face new intergenerational conflicts. And we conceive of our own lives not as a single duration but as a sequence of many possible lives. As the economist Hervé Juvin has remarked, “Aging is becoming a social phenomenon rather than a physical one.”2
While modernity’s idea of progress was tied to general cultural, moral, economic, and material advancement, today progress is concentrated in the improved performance of individual bodies.3 Pursuit of the “good life” in the twenty-first century is a quest for pleasure, attainable through various available modes of consumption. This finds its fullest expression at a certain period in our lives—the “golden years” of retirement, when we are free of the constraints of family and work but are not yet eroded by the body’s deterioration. At this age, we live permanently at leisure, fulfilling both the utopian visions of the 1960s avant-garde and an ideal consumerism. And like all utopian visions, that of the American and European residential retirement community, too, depends on certain degrees of segregation.
The medicalization of our society has initiated a process in which the nonmedical problems of daily life (from anxiety to infertility, from aging to death) are more and more treated as medical. And according to Peter Conrad, “The key of medicalization is definition. That is a problem is defined in medical terms, described using medical languages, understood through the adoption of a medical framework, or ‘treated’ with a medical intervention.”4 Architecture and urban planning have since undergone a parallel process; they rely increasingly on medical rhetoric to describe problems and arrive at solutions defined in the medical milieu. An ever-increasing number of urban, environmental, and architectural problems are treated as medical, and remedies are sought in increasingly specific solutions. Tailoring requirements to particular groups of ill, or presumably ill, individuals leads to conflicting, contradictory solutions, and finally to the even greater segregation of various demographic groups. In this sense, architecture—subject to medicalization—should itself be considered a “sick” body.
Architecture and urban planning have adopted the bellicose stance of Western medical rhetoric, aiming to “combat” illnesses, viruses, and stress. Other attitudes have been neglected, such as the simple activity of listening, which homeopathic specialist and entrepreneur Christian Boiron considers fundamental for understanding the real crises of which “illnesses” are only a symptom. Or Nan Ellin’s suggestion for a process of improvement based on potential present within a territory, rather than the notion of treatment.
Nevertheless, medicalization remains a bidirectional process. Though it can be described as a phenomenon of incremental development, having occurred in our society during the last century, the reverse process is still possible. And demedicalization has successfully occurred in some cases, for example with regard to homosexuality and masturbation.5
The demedicalization process, if applied to architecture, might allow the discipline to escape the ambiguity and moralism of contemporary ideas of health by taking both problems and solutions out of the realm of individual commitment and restoring them more appropriately to social surroundings. In this way, it might be possible to recover one’s capacity to be critical with respect to public health policies; to take part in the debate while renouncing the allegedly rational, scientific solutions prescribed by a medical idea of health. As architects Kersten Geers and David Van Severen observe in their theoretical project for a healthy city, the most significant shift for architecture and urbanism will be from the idea of cure to the idea of care—in the process of taking care of our bodies and our environments.
This text is excerpted from the introduction to Imperfect Health, a book that accompanied our 2011 exhibition of the same name.